No joke: Glenohumeral joint arthritis and rotator cuff tear increases need for revision of total shoulder replacements
Surgical replacement of the shoulder joint is an increasingly common procedure.[1] Though less prevalent than knee or hip replacement, total shoulder arthroplasty (“TSA”) purportedly improves ranges of motion and provides relief from debilitating joint pain.[2]
Review of the prevailing scientific research reported in the Journal of Bone and Joint Surgery reveals glenohumeral[3] osteoarthritis and rotator cuff tears increase the likelihood of TSA revision.[4]
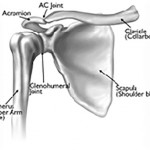
The shoulder joint is a ball-and-socket structure, comprised of three bones: Scapula (shoulder blade), Clavicle (collar bone), and Humerus (upper arm). The “ball” of upper end or head of the humerus bone fits snuggly into the glenoid bone, concave “socket” cavity of the scapula. The articular surfaces[5] are covered with cartilage that reduces friction and eases joint movement.
Osteoarthritis is age-related “wear and tear” that softens and deteriorates the protective layer of cartilage and underlying bone. Progressive loss of cartilage and resultant bone-on-bone produces joint stiffness and pain. When conservative measures such as a course of anti-inflammatory agents and physical therapy fail to adequately reduce symptoms, arthroplasty – surgical replacement of the shoulder joint with an artificial prosthetic – successful reduces pain and increases function.
Medical research reveals post-surgical arthritic changes in the glenoid bone or rotator cuff tears cause misalignments that change the force vectors of the ball-and-socket prosthetic. The altered forces may lead to accelerated wear of the implant, component loosening, prosthetic shoulder joint instability, and increased pain. Further surgery, including complete redo or revision, may be required.
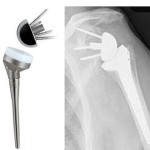
Reverse Shoulder Joint Prosthesis: The “ball” is at the shoulder blade. The “socket” is at the head of the upper arm.
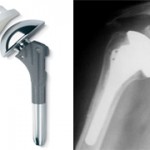
Standard Shoulder Joint Prosthesis: The “ball” is at the top of the upper arm bone. The “socket” is at the shoulder blade.
The literature suggests a “reverse” TSA may be appropriate in cases of significant osteoarthritis with bone loss and rotator cuff tears that alter the glenohumeral mechanics. Reverse TSA reportedly offers improved fixation and stability over replacement with a standard anatomical prosthesis.
The study notes high complication rates for reverse TSA. Post-surgical recovery difficulties may be due, in part, to the severity of underlying osteoarthritis, ligamentous instability, and relative surgical inexperience with the procedure.
Employers, insurers, and their workers’ compensation administrators should take note of the medical research. The claim file should contain specific information prior to authorizing TSA. Specifically, the claims manager should obtain a full diagnostic assessment of the nature and extent of any degenerative glenoid bone loss, the severity of rotator cuff tendon tears, and a prognosis of the likelihood of post-surgical prosthetic instability. The claims manager should also make appropriate inquiry of the surgeon’s experience if a reverse TSA is recommended.
Should you have any questions regarding the efficacy or coverage of standard or reverse total shoulder arthroplasty, please contact one of our attorneys.
[1] 10,000 Total Shoulder Arthroplasties in 1990; 20,000 in 2000; and 53,000 in 2011, American Academy of Orthopaedic Surgeons, (See web site: www.aaos.org/wordhtml/research/stats/arthropl.htm.)
[2] More than 900,000 Americans have total hip or knee arthroplasties each year. Waiter, J. Michael, “Shoulder Joint Replacement,” OrthoInfo, American Academy of Orthopaedic Surgeons, December 2011. (See web site: //orthoinfo.aaos.org/topic.cfm?topic=A00094)
[3] The glenohumeral joint is the “ball-and-socket” of the shoulder.
[4] Stephens, Scott P., et al., “Shoulder Arthroplasty in the Presence of Posterior Glenoid Bone Loss,” J Bone Joint Surg Am, 2015; 97:251 (Feb 4, 2015) (“The loss of posterior glenoid bone can alter joint reactive forces, resulting in humeral head displacement sand eccentric stresses placed on the glenoid component. This may lead to polyethylene wear, component loosening, or instability. Loss of posterior glenoid bone results in the net humeral joint reaction forces passing outside the effective glenoid arc, creating joint instability.”)
[5] The articular surface is the point of contact between two bones or cartilage.